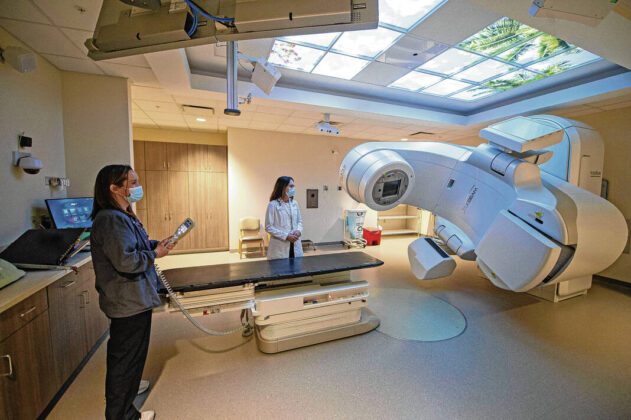
Doctors with the Sue Ann Wortman Cancer Center at Hancock Regional Hospital; from left; Stephen Schultz, MD; Julia Compton, MD; Jolyn Veza, NP; Namrata Shah, MD; and Pricilla Stumpf, MD. Tuesday, April 27, 2022.
Tom Russo | Daily Reporter
GREENFIELD – For most of his 37-year career as an oncologist, Dr. Stephen Schultz would look around staff meetings and see mostly middle-aged white men like himself in the room.
Today, he’s the only man working with a team of three female oncologists and one female nurse practitioner – all in their late 30 and early 40s – at the Sue Ann Wortman Cancer Center in Greenfield.
The predominantly female, younger-than-average staff is a sign of the times in the changing medical world, but it’s still a bit of an anomaly in a field long-dominated by men.
“The average age of oncologists is around 47, and about 55% to 65% are women,” said Dr. Julia Compton, who directs the staff at the Greenfield cancer treatment center.
Compton helped lead the charge in opening the center in 2015 and was tasked with hiring a staff of the best oncologists she could find.
She set about to do just that through a nationwide search. It just so happened she hired mostly physicians similar to herself – young moms looking to provide the very best patient care while maintaining a healthy work-life balance.
“We were looking for doctors who were extremely talented but who would also fit our culture here at Hancock, and part of that culture is that we prioritize work-life balance. All of us work three to four days a week, which allows for that balance as well as a team-based approach to providing patient care,” said Compton, who is the mother of three children ages 3, 6 and 8.
While Schultz’s children are grown, all the other members of the cancer center team have young kids at home, including Dr. Namrata Shah, Dr. Priscilla Stumpf and nurse practitioner Jolyn Veza.
“Having that sense of balance is essential,” said Stumpf, who worked at the University of Colorado before joining the cancer center staff last summer.
“I have four kids 5 and under, and we’re firing on all cylinders every day, trying to make it from one nap time to the next,” she said with a laugh, taking a quick break with her colleagues at the center Tuesday afternoon.
Stumpf said the fact that the center’s overseeing body, Hancock Health, prioritizes a healthy work-life balance was a big part of why she was drawn to work there.
“Hancock was really willing to work with me, which was a huge help,” she said.
Compton said the shift toward offering healthcare providers a flexible schedule has paved the way for physicians, especially women, to enjoy the best of both worlds – making it easier to raise a family while building a rewarding career.
“If you think back, it used to be that there was a single working parent in the house, which was typically the man, but what you see more now is two working parents,” she said.
“The old way wasn’t typically conducive to women working in medicine because it was very difficult to co-parent while working full time. Now you’re seeing more women in healthcare than you ever have before because there’s this ability to co-parent from home and share responsibilities.”
That culture is somewhat unique in the medical field, said Compton, especially in the demanding field of oncology.
Shah, who joined the cancer center in January, said a healthy work-life balance is essential for all physicians, regardless of age or gender.
“Oncology is a challenging field, caring for patients who are actively fighting for their lives,” she said. “I think every oncologist should have a four-day work week, whether they have young kids at home or not.”
Stumpf said striking that healthy balance allows physicians to give fully of themselves, both at work and at home.
“That balance allows me to focus on my family while I’m at home, so that when I come to work I can be laser-focused on my patients,” she said. “We can leave all the emotional and physical stress of being a young parent at the doorstep when we come to work, so we can bring that energy to care for our patients with fresh eyes.”
Schultz said he and his wife relied on a nanny to help out when their children were young, since both parents worked full time.
The seasoned physician is thrilled to see the medical field changing to be more accommodating to young families’ needs.
He’s also happy to see the cultural changes paving the way for more women to enter the medical field, especially the field of oncology.
“I think there’s a lot of benefits to diversity among us physicians, especially when it pertains to cancers of the female system. We take care of women, and women very often want women oncologists,” he said.
Veza has found that to be true in her work as an oncology nurse practitioner.
“Especially with breast cancer and those types of diagnoses, a lot of times women are more comfortable with receiving care from women healthcare providers,” she said. “I think when you can relate to someone with what they’re going through as a female, it can affect the kind of care you provide.”
Schultz said the problem is a nationwide shortage of oncologists, which is projected to only worsen as the population ages and increases the demand for care.
According to The Oncology Group, a nationwide team of cancer care advisors, a recent study by the American Society of Clinical Oncology projected shortage of medical and radiation oncologists through 2025.
The study showed that changes in prevention and screening guidelines, along with physician retirement rates, would help contribute to the overall offset, which was estimated to be a 40% increase in demand and a 25% increase in supply.
Stumpf said she’s thrilled to see more women joining the ranks of medical school students and physicians nationwide, a trend she hopes will continue indefinitely.